Symmastia means the abnormal position of the breasts, breast prostheses, the confluence of the breasts in the midline or positioning of one of the breasts towards the midline of the chest. In some cases, prostheses may appear as combined by displacing and joining in the chest.
This condition may develop due to the formation of a very large space for prosthesis during the surgery, and in particular by creating a large space in the middle of the chest cage. Often, this may occur with prostheses placed under the muscles, but sometimes even with prostheses placed on the muscles.
Previously, the only and best way to correct this was to remove the prostheses and wait for months to heal. Then, in a single session, new prostheses were placed in their new spaces.
Years ago, scientific articles were written on how to correct this situation and the term “capsular contracture” repair was proposed. This term essentially means using the suture to close the cavity close to the middle area and to apply it to both sides and then to replace prostheses at the same time.
In solving this problem, this method was a more primitive procedure; there were times when it worked, but it was a difficult technique to apply surgically and was not popular. If prostheses were on the muscle, they could be replaced under the muscle to correct the problem. However, since the problem usually arises with sub-muscular prostheses, it is not applicable to most patients.
Recently, many surgeons have begun to apply a new surgical technique that is both easier and safer to overcome this problem. This procedure is called a neosubpectoral pocket or new sub-muscular pocket. Essentially, this operation allowed us to create a new pocket for prostheses by closing the old pocket at the same time. However, in this case, with the repair of the capsule, instead of partially closing the old pocket, we close it completely.
With this surgery, it is possible to solve not only symmastia but also many prosthetic displacement problems and even in some cases, the capsular contracture. This method, which requires an advanced planning and application, is successfully applied by surgeons with a breast reconstruction experience. We also successfully perform these surgeries in our clinic with more than 15 years of breast reconstruction experience.
Even In recent years, we have been able to increase the chances of success by introducing materials such as Acellular Dermal Matrix (specially treated cadaveric skin) or artificial skin to support and reinforce these repairs. Just as the chimney skirt protects the chimney from the leakage of the metal dropper, the artificial skin gives us the opportunity of treatment by using a neosubpectoral pocket and then to strengthen and support with the artificial skin.
In many cases, we use tissue-based patches or artificial cadaveric skin. Recently, however, surgeons have started using biological fascia and synthetic Vicryl mesh instead of tissue-based patches.
In addition to the surgical treatment that can be performed almost always in a single step instead of waiting for a period of time after the removal of prostheses, we usually recommend that you choose a prosthesis that will probably fit better or fill the cavity, which means a smaller prosthesis than the original one. Not always, but in some cases, the problem is not caused by repeated entries to the tissue or the creation of new pockets, but also it may be due to the fact that initial prostheses were large for the female anatomy or the size of the chest cage.
Although the development and diagnosis of symmastia is a disappointing experience for a woman with breast prosthesis, the good news is that experienced surgeons have a chance to safely treat it by means of appropriate methods as described above.
You should try to find self-confident surgeons with a high level of experience and expertise in breast reconstruction to solve this problem.





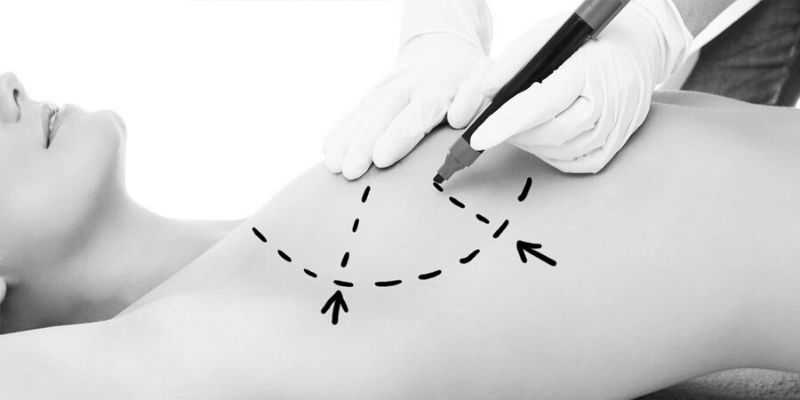



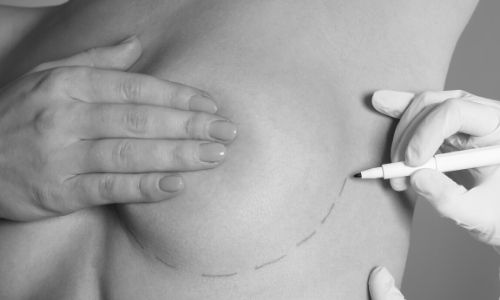




Hi
I had breast cancer In 2019, chemotherapy, mastectomy, radiotherapy, L DIEP flap, breast expander and a silicon implant in the right breast and left breast reduction, this was done in august 2022. This was done by the nhs in England. Unfortunately this has left me with a high riding right breast and the pectoralis muscle is very noticeable. Im very conscious of this. The nhs surgeon has talked about possibly removing the silicone annd the muscle and fat grafting or using the tummy to do a flap. But there is a long waiting list and this might not be done for another year. I can’t wait that long as it’s affecting my confidence so I realise I have to look into having this done privately.
Hello,
We can organize a meeting with the doctor for examinations and surgeries. You can ask him all the details you are curious about during the interview. You can contact [email protected] from our e-mail address for an appointment.
Hello,
Can the doctor reconstruct the breast with fat grafting alone (no flap)? I have all my own skin. I had a skin and nipple-sparing mastectomy so my skin is there like a breast envelope with an implant I want removed and replaced with my own fat. Does he do that? Thank you!
Hello,
We can organize a meeting with the doctor for treatment and surgeries. You can ask him all the details you are curious about during the meeting. You can contact [email protected] from our e-mail address for an appointment.